U.S. facing worst flu season since 2009, experts say
Input
Changed
The Growing Threat: Hospitalizations and Rising Death Toll Government Response and Vaccine Distribution A Changing Landscape: The Political Divide and Health Policy
In a startling development, the U.S. is currently facing its worst flu season since 2009, with experts sounding alarms about the severity of the outbreak. Despite COVID-19 dominating headlines in the past few years, influenza has once again emerged as a major health threat, causing widespread illness, hospitalizations, and an unsettling number of deaths. The flu season of 2025 has already been marked by a troubling increase in cases, leaving experts and healthcare professionals scrambling to manage the situation. For many, the similarities between this year’s flu crisis and the COVID-19 pandemic are hard to ignore.
The Growing Threat: Hospitalizations and Rising Death Toll
The 2025 flu season has been unlike any other in recent memory, with reports indicating that it has surpassed previous years in terms of both cases and fatalities. According to health experts, this season is officially the worst since 2009, when the swine flu (H1N1) pandemic took the world by storm. The current surge in flu cases is strikingly similar to the intensity of the COVID-19 pandemic, leaving some wondering if this could signal the beginning of another public health crisis.
While the Centers for Disease Control and Prevention (CDC) had initially raised concerns over a potential flu outbreak in January, it is only in the past few weeks that the situation has spiraled out of control. The agency recently reported that flu-related deaths have exceeded those caused by COVID-19, a development that has caught many off guard. For many Americans, it is a harsh reminder that pandemics and viral outbreaks are not a thing of the past. The ongoing flu crisis underscores the delicate balance that public health authorities must strike between monitoring various threats and ensuring that appropriate interventions are in place to contain the spread of disease.
As of mid-February, the number of flu-related hospitalizations has reached record levels across the U.S. Over 100,000 Americans have been admitted to hospitals, a number that continues to climb by the day. What is most concerning is the demographic of patients most severely affected. Unlike COVID-19, which primarily impacted older adults and those with underlying conditions, this flu season has affected a broader swath of the population, including young adults and children.
In many states, hospitals have reported overwhelming emergency room visits, with some regions seeing a shortage of available beds and healthcare staff to manage the surge. Health officials have raised concerns that flu cases will continue to overwhelm the healthcare system in the coming weeks, especially as flu season typically peaks between December and March. The CDC has urged the public to seek medical attention if they experience symptoms such as fever, cough, and shortness of breath, as early intervention can help prevent severe complications.
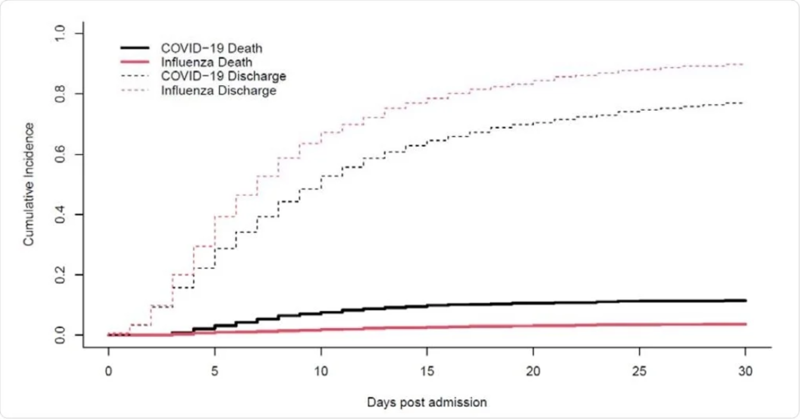
In an even more alarming development, flu-related deaths have outpaced those attributed to COVID-19. This is particularly concerning given that, since the emergence of the COVID-19 pandemic, many had hoped that viral outbreaks like the flu would become less dangerous. However, the flu’s resurgence has shattered those hopes, highlighting that the U.S. is still vulnerable to the ongoing threat of infectious diseases.

Government Response and Vaccine Distribution
At the heart of the current crisis lies the issue of vaccination. While the CDC recommended an annual flu vaccine for all Americans, vaccination rates have remained relatively stagnant. Despite the availability of flu vaccines, the public's reluctance to get vaccinated has become a significant barrier to preventing the spread of the virus. According to reports from the CDC, only around 40% of the population has received the flu vaccine this season—far below the threshold needed for herd immunity.
What has further complicated the vaccination effort is the vocal opposition to vaccines from certain political figures. The recent appointment of RFK Jr. as the Secretary of Health, a staunch critic of vaccine mandates, has caused a stir in public health circles. RFK Jr.’s views on vaccines are well-documented; he has long argued that vaccine safety is not fully understood and has advocated for more rigorous testing and regulations. While his statements have been controversial, his appointment to such a high-profile position raises significant concerns about the potential erosion of trust in public health initiatives.
RFK Jr.’s counter-narrative has made it more difficult for the CDC and other health agencies to promote widespread vaccination efforts, especially when it comes to flu shots. In a time when the public is already wary of vaccine-related misinformation, having a prominent figure publicly question the safety and efficacy of vaccines has only fueled skepticism. This is particularly troubling in the midst of a severe flu season when vaccines could have prevented many cases of serious illness and death.
The U.S. government’s response to the current flu outbreak has been a point of contention. Public health officials argue that the government could have done more to prepare for this flu season. Unlike the COVID-19 pandemic, for which the government ramped up vaccine production and distribution efforts at an unprecedented scale, flu vaccines have not been distributed with the same urgency. While flu vaccines are available annually, there has not been the same level of mobilization to ensure that every American gets vaccinated, particularly in underserved and vulnerable communities.
Furthermore, experts argue that the government should have been more proactive in anticipating the scale of the flu outbreak. While some regions saw warning signs of a potential flu surge, a lack of preparedness meant that many hospitals and healthcare facilities were overwhelmed when the cases began to rise. This lack of foresight is exacerbated by political infighting, particularly as the new administration, led by President Trump’s appointee RFK Jr., has faced challenges in promoting public health initiatives.
This lack of action in the face of an obvious threat has caused many to question the current administration’s commitment to safeguarding public health. If the government had been more proactive in its vaccine distribution and public health campaigns, many of the cases and fatalities seen today could have been prevented. Furthermore, the absence of strong political leadership on vaccine advocacy has made it difficult to build public trust in the necessary measures to combat the outbreak.
A Changing Landscape: The Political Divide and Health Policy
The ongoing flu crisis has also highlighted the political divide in the U.S. when it comes to public health policy. The intersection of politics and healthcare has never been more apparent than it is today, as vaccine hesitancy and skepticism have become entrenched political issues. What is particularly concerning is how political figures, such as RFK Jr., are using their platforms to oppose vaccination policies, which undermines the efforts of public health officials trying to contain the flu.
The political debate surrounding vaccines is not new, but it has become more pronounced in recent years. The backlash against vaccine mandates, combined with political figures who question the efficacy and safety of vaccines, has made it harder for public health officials to carry out their mission. It is clear that, moving forward, political willpower will be a key factor in determining the success of the government’s efforts to address public health crises.
As the U.S. grapples with its worst flu season since 2009, it is becoming increasingly clear that a more coordinated and effective response is needed. Public health measures, such as vaccination, need to be treated with the same urgency and importance as those deployed during the COVID-19 pandemic. Additionally, stronger leadership and bipartisan support for vaccine initiatives are essential to avoid further health crises in the future.
Ultimately, the U.S. must learn from its experience with the flu season of 2025. This outbreak has served as a reminder that viruses, even those as common as the flu, can have devastating effects on public health when proper precautions are not taken. Moving forward, the government must prioritize preparedness, vaccination, and public health leadership to ensure that future outbreaks are better managed and mitigated.





















